RHEGED | Health Issues That May Effect ESS

First & foremost, it is pleasing to note that English Springer Spaniels (ESS) are not troubled in general by serious health problems, other than some of the more usual canine illnesses & infectious diseases that can affect the whole canine population.
Any visible physical changes that have taken place over the 100 years since the Breed was recognised by the 'Kennel Club', have not been recorded as being, for the most part, detrimental to the Breed's health & welfare.
Hereditary (inherited) diseases known to exist in the ESS are not thankfully widespread. However, if you would like to know more about what health & welfare issues the Breed is tackling, & how you might be able to better understand them, please read on.
It is best to use common sense & caution whether breeding with, or looking to purchase, an ESS, from whatever source, as not all conditions that can affect the Breed will have tests that can predetermine the outcome to the health & welfare of the ESS puppies that are produced.
For further information ~ RHEGED | Understanding Genetics & Test Results page
PHOSPHOFRUCTOKINASE DEFICIENCY (PFK)
WHAT IS IT?
Phosphofructokinase (PFK) is a major regulatory enzyme found in all cells of the body, which catalyses (stimulates by means of a chemical reaction) the metabolism (conversion) of sugar into energy to maintain normal cell function. PFK deficiency is an enzyme storage disease which causes abnormalities in red blood cells & muscle cells. It is inherited in English Springer Spaniels through a single autosomal recessive trait.
TREATMENT
It is essential to get a proper diagnosis, as PFK deficiency can sometimes be confused with autoimmune haemolytic anaemia & other acquired diseases. Clinical manifestations usually resolve within hours to days. While there is NO actual treatment for PKF, it can be successfully managed to the point that affected dogs may have a relatively normal lifespan. The most important "treatment" is managing the dog's activity & stress levels, to prevent more severe anaemia. Situations that can precipitate such crises (including strenuous exercise or stress) should be avoided. In cases where anaemia becomes critical, veterinary care is required to manage the condition until it normalises.
A tiny change (point mutation) in the M-type phosphofructokinase gene was identified by research groups at the University of Pennsylvania, which has resulted in the availability of a genetic screening (DNA) test for PFK deficiency. This DNA test accurately determines whether an ESS is affected, a carrier, or a normal dog.
| CANINE FUCOSIDOSIS (FS) IS SEVERE, PROGRESSIVE & ULTIMATELY FATAL. TESTING IS IMPORTANT. IT CAN AFFECT ALL ENGLISH SPRINGERS, WHETHER THEY HAVE BEEN BRED FOR FIELD TRIALS, WORK, SHOW OR AS A COMPANION. DO NOT LET ANYONE TELL YOU OTHERWISE! |
A DNA test has been available since 1997 & can be undertaken at any age and needs only to be done once in a dog's lifetime, making it safe, for the time being at least, for the breed to use identified Carriers. The condition is inherited through an autosomal recessive trait and has been reported by ESS owners & breeders from all over the world.
It is characterised by deteriorating signs of the nervous system that progress over a period of several months, sometimes from an early age. Signs include inco-ordination & ataxia (loss of control of movement), change in temperament, loss of learned behaviour, loss of balance, apparent deafness, visual impairment & varying degrees of depression. The inco-ordination & ataxia affects all 4 legs & is mostly evident when affected animals are walking on slippery surfaces or attempt more complicated movements such as turning. In addition, affected dogs lose weight & may suffer from swallowing difficulties & sometimes regurgitation of food.
- A Kennel Club Breed Scheme for Fucosidosis has been in operation since 2005, with results now recorded in the KC's Quarterly Breed Records Supplements, on KC Registration documents & on the KC's Website, thus ensuring that the audit trail of information about a ‘genetically clear' for Fucosidosis English Springer is not lost.
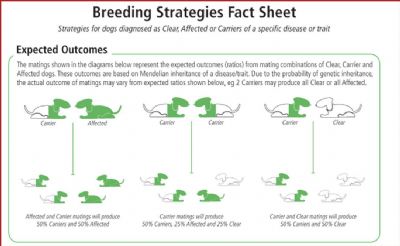
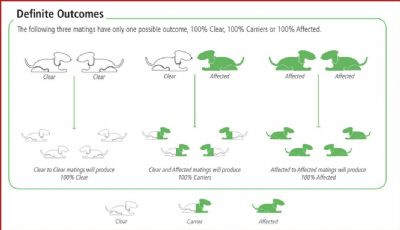
- ESS Breeders can plan their breeding programmes accordingly, making it feasible to completely eradicate this fatal disease from the Breed. For the time being, should they wish to use a CARRIER in order not to sacrifice excellent breed points, this is OK provided it is NEVER mated to another CARRIER or to an UNTESTED dog. Likewise, 2 untested dogs (unless from genetically clear parents) should never be mated together.
- By mating a CARRIER to a CLEAR, we will not be producing AFFECTED dogs ~ we will just be prolonging the production of CARRIERS. Although not an ideal situation, it is acceptable until breeders find the ‘Clear' dog that also proves to be their ideal stock to carry on their breeding lines.
PROGRESSIVE RETINAL ATOPHY (PRA)
SUB CLASSIFICATIONS OF PRA:
Primarily affects the photoreceptor (light sensitive) cells. Both eyes are similarly affected (bi-lateral) & dogs eventually become totally blind. It is regarded, in the English Springer Spaniel, as being a late onset (4 ~ 5 years) condition, but it can appear as early as 2 years of age.
- CORD1 MUTATION:
In 2007, researchers announced that agene mutation (known as the CORD1 Mutation) had been identified as a major risk factor for the development of specific form of PRA in English Springer Spaniels. A DNA test for this mutation has been developed & is not available in Australia, the USA & the UK. Following the instroduction in 2008 of a Kennel Club (UK) Breed Scheme for the PRA Cord 1 mutation, ESS owners & breeders are encouraged to use the DNA testa available. Other forms of PRA that may also exsist in the breed have not yet been genetically identified & cna only be therefore be deteced by clinical eye testing.
As it would appear that there are other mutations in the English Springer Spaniel that are causing PRA (other than Cord 1), it is vital that blood samples/cheek swabs from any ESS that are clinically diagnosed as affected (but are not genetically affected for the Cord 1 mutation) are submitted to the appropriate authorities to assist in further studies of canine PRA.
- CENTRALISED (CPRA) RETINAL PIGMENT EPITHELAIL DYSTROPHY (RPED):
The abnormality is in the retinal pigmented epithelium (RPE). The photoreceptor cells will also degenerate eventually. The rate of vision loss is much slower than with generalised PRA, & not all dogs become totally blind. Detectable between the ages of 12 ~ 18 months by clinical eye examination.
Primary Glaucoma in English Springer Spaniels is an inherited condition, also known as 'Angle Closure Glaucoma'. It usually begins in 1 eye, but almost always eventually involves both eyes, leading to complete blindness. Abnormal drainage of the eye's aqueous fluid leads to the pressure inside the eye rising to double or treble its normal value. The increased pressure destroys cells within the retina, & this can happen so quickly that often treatment is too late to restore eyesight. It is characterised by sudden onset blindness & pain, & such is the damage that removal of the eye may prove necessary in many instances.
THE ONSET OF GLAUCOMA IS A MEDICAL EMERGENCY
A condition called Goniodysgenesis, in which dogs are born with a narrowing of the iridocorneal angle (the angle at which the iris and cornea join), is known to be a major risk factor for the development of Primary Glaucoma. Veterinary Ophthalmologists use an eye test called 'gonioscopy' to identify those dogs that may be predisposed to the development of Primary Glaucoma. This test involves placing a special contact lens directly onto the surface of the eye which allows examination of the drainage angle. Gonioscopy is a one off test, & screening can be carried out on dogs from the age of 4 months onwards.
Retinal dysplasia is an eye disease affecting the retina & is usually non progressive. As well as a genetic defect, it can be caused by a viral infection, drugs, or Vitamin A deficiency. It is characterised by folds or rosettes (round clumps) of the retinal tissue. Retinal dysplasia can be focal, multifocal or geographic, or accompanied by retinal detachment (causing blindness).
Breeders are advised to avoid using ESS affected with this condition in their breeding programmes.
WHAT IS IT?
For further information ~ Hip Dysplasia fact sheet (PDF)
WHAT DOES A NORMAL HIP LOOK LIKE?
In the normal anatomy of the hip joint, the femur (thigh bone) is connected to the pelvis at the hip joint. The almost spherical (rounded) end of the femur head fits into a concave (curved in/hollow) socket (acetabulum) located in the pelvis. The bony surface of the femur head & of the acetabulum is covered by cartilage. While bones provide the strength necessary to support body weight, cartilage ensures a smooth fit & a wide range of motion. Normal hip function can be affected by congenital (present since birth) conditions such as dysplasia, by trauma (injury), & by acquired diseases such as arthritis.
HOW DO I FIND OUT IF MY DOG HAS HD?
If your dog should show signs of stiffness or soreness after rising from rest, reluctance to exercise, bunny-hopping or other abnormal movement, lameness, pain, reluctance to stand on it's rear legs, jump up, or climb stairs, he/she might be suffering from Hip Dysplasia, please visit your Vet for a consultation for a proper confirmation of a diagnosis for HD.
Your Vet might suggest the use of X- ray to confirm the presence of hip dysplasia. Often the animal will be anaesthetised or sedated to achieve clear diagnostic results. Since the condition is to a large degree inherited, it is important to consider making sure that the hip scores of parents are professionally checked.
Radiographic (X-ray) features may not be present until 2 years of age in some dogs. Whilst many affected dogs do not initially show clinical signs, some dogs manifest the problem at an early age, with others not showing it until well into adulthood. The minimum age of the dog at the time of the hip X-ray is 12 months; there is no upper age limit. Dogs may not be scored under present schemes more than once.
A dog may have good X-rays & yet be in pain, or may have very poor X-rays & apparently almost no problems. The hip condition is only 1 factor to determine the extent to which dysplasia is causing pain or affecting the quality of life. In mild to moderate dysplasia it is often the secondary effects of abnormal wear & tear or arthritis, rather than dysplasia itself, which is the direct causes of visible problems.The underlying hip problem may be mild or severe, may be worsening or stable, & the body may be more or less able to keep the joint in repair well enough to cope. Different animals have different pain tolerances & different weights, & use their bodies differently, so a light dog that only walks will have a different joint use than a heavier or very active dog.
Each case must be treated on its own merits, so this is why it is important that you consult with your Vet at the earliest opportunity, if you are having any concerns. Please note that, despite the fact that the condition is inherited, it can occasionally arise even in animals with impeccable hip scored parents. Therefore, there is good reason to keep track of current genetic research in this area (the chance to establish a DNA test for example).
WHAT IS THE TREATMENT?
The bad news is that there is no total cure, but the good news is that there many options available to alleviate the clinical signs, often with the use of drugs, such as non steroidal anti inflammatory (NSAID) (e.g Rimadyl and Metacam). Let your Vet be the best judge of what drugs best suit your dog & its symptoms. It might also be the choice of your Vet to select the use of a glucosamine based nutritional supplements to give the body additional raw materials used for natural joint repair.
- There are also currently several products on the market to help dogs suffering from HD to help them get around better (pressure reducing beds, ramps) or even the specialised treatments such as Hydrotherapy.
- Watching the weight of your dog, its feeding & exercise schedule, should all be kept in equal balance, as it is vital to help alleviate the symptoms &/or the onset of arthritis. Reasonable exercise can stimulate cartilage growth and reduce degeneration.
ARE THERE OTHER CONDITIONS WHICH CAN MIMIC/REPLICATE HD SYMTEMS?
Yes, there are, which is why it is so important that you consult a Vet for a proper diagnosis to provide you with specific clinical evidence. Any dog may misuse its rear legs, or adapt its gait to compensate for a pain in the forelegs, hocks, stifles or spinal area.
Other conditions, such as cranial (anterior) cruciate ligament tears, where usually the dog holds its affected leg up (which is unusual with HD) or other rear limb arthritic conditions can also be masked by mild dysplasia.
WHAT IS IT?
For further information ~ Epilepsy fact sheet (PDF)
For further information ~ Canine Epilepsy Research
The word EPILEPSY refers to repeated seizures ('fit' or convulsion) caused by excess electrical activity in the brain, which disrupts the normal communication between brain cells. The seizures indicate a sign of brain disease or disorder, much like a cough might be a sign of lung disease. In any event, it is a sign of a problem which unfortunately is usually not going to go away without further close investigation &/or treatment.
Epilepsy is one of the most common neurologic diseases in dogs. It is the tendency for the disorder to be so unpredictable that makes it such a complex disease with which to deal. A seizure may occur as a one off event from a variety of causes, but it is only if seizures repeat again & again over a period of time that it is called epilepsy.
Seizures are caused by excitatory influences on nerve cells in the brain, although there can be other causes that might tip the balance from inhibition towards too much excitation in the brain. It has nothing to do with the dog's emotional state, so any animal might 'fit' if pushed past that threshold of electrical stimulation. Other influences that may cause a seizure might be toxins (poisonous plants, chemicals & insecticides), metabolic disease (low blood sugar or heart disease) & direct damage to the brain (injury or tumour).
Seizures are divided broadly into 2 types: generalised & focal (or partial). Generalised is where the electrical storm in the brain arises everywhere at once. In a focal or partial seizure, the abnormal electrical activity arises in a small area of the brain only.
The most common time for a dog to have a seizure is when it is relaxed & quiet. In some instances, the dog can actually be sound asleep. However, seizures can occur at any time, but should they occur when the dog is exercising or excited, your Vet may look for another cause such a heart problem or low blood sugar.
- The first phase is known as the 'aura' or prodromal stage, which is the time when there is the earliest sign of a recognisable change in the dog's behaviour. This can alert the owner to an impending seizure. However, some dogs do not show aura, with the seizure coming out of the blue.The dog is likely at this stage to show confusion, fear, rage or even seek attention or withdraw from his owner & hide (the 'tonic' stage).The classic seizure (tonic ~ clonic) begins with motor activity (rigid or jerky muscle spasms or paddling). Once the seizure has begun the animal will fall to its side with legs outstretched & head back & may also lose consciousness, even though its eyes appear to be open. This will be accompanied by autonomic activity (salivation, urination & defecation). Changes in sensory function may lead to pawing at the face, tail chasing, or biting at part of the body or the air.
It is important that during the 'clonic' phase of the seizure, the owner ensures that all other pets & children are kept out of the way. Other than to give the dog plenty of space, make certain the dog is safe ~ that it cannot fall down the stairs, bang into a sharp edge, get tangled in an electric cord or otherwise cause injury to itself. It is not necessary to do anything, but keep a close eye on what is happening & keep a note of the time it takes for the seizure to abate.
|
THE DOG WILL NOT SWALLOW ITS TONGUE, SO PLEASE
KEEP YOUR HANDS AWAY FROM ITS MOUTH. Without a doubt, this is the most distressing time for the owner, as a seizure can often be both frightening to watch and emotionally overwhelming. |
Most seizures are brief & isolated but seizures can come in clusters where the dog has a 'fit', recovers, & then immediately has another seizure. This could be the danger point for a dog to lapse into a continuous seizure requiring urgent & immediate medical attention. Any seizure lasting longer than 30 minutes is likely to cause the dog to fall into a coma or to cause serious brain damage. The seizure creates a tremendous stress on the heart & other organs, with the body temperature rising as a result of all the muscle activity.
HOW EPILEPSY IS DIAGNOSED?
Early evidence of epilepsy is usually seen within the first 3 years of a dog's life & it is acknowledged that several breeds (including the English Springer Spaniel) can be predisposed to develop the condition. After this age, the seizures are more likely to be caused by an active disease process, such as infection, trauma, metabolic disorder or a tumour.
HOW IS EPILEPSY TREATED?
Treatment depends on factors such as the severity & frequency of the seizures. Regular medication is used to control the seizures, with Phenobarbital being the drug most commonly used, as it is safe, effective & inexpensive.
Diazepam (valium) is also an effective drug used in the treatment of epilepsy, but if it is given daily there is always the possibility of it losing its effectiveness. Therefore, it is usually reserved for administration to the dog during a seizure, in the hope of arresting it. It is given to the dog during an active seizure either by intravenous injection or more usually by suppository (per rectum). This has proved particularly helpful as a preventative treatment for dogs having cluster fits.
IS THERE ANY EVIDENCE TO INDICATE THAT EPILEPSY IS INHERITED?
Unfortunately, many of the idiopathic epileptics will have a form of inherited epilepsy caused by a mutation in a specific gene, which has been inherited from their parents. The mode of inheritance is as yet unknown & will vary between breeds, & in fact it could be that more than one gene is involved.
WHAT HELP OR SUPPORT IS AVAILABLE?
- Try to plan ahead as best as you can to make sure that in the event of a seizure your dog is safe from hurting himself.
- Keep calm & relaxed as best you can at all times, to convey to your dog that you are in control & he has nothing to worry about.
- Do not stop having fun with your dog. Most epileptic dogs can live relatively normal lives, although requiring daily medication to control their condition.
- Always make sure you have enough medication available (especially if you are away from home, or have left the dog in someone else's care, public holidays etc)
- Feed a high quality balanced diet to suit your dog's needs & which is in balance with the amount of exercise he is taking.
- A weak or defective immune system fails to protect the body, leaving it vulnerable & open to attack by an opportunistic infection.
- A dog with an autoimmune disease does not have a ‘weakened' immune system. On the contrary, it works extremely well ~ but what it does have is a confused one, whereby it begins to attack & reject the body's own tissue as foreign.
- A genetic predisposition in certain breeds (including the English Springer Spaniel)
- Multivalent modified live vaccines & some drugs (which can over stimulate the immune system)
- Environmental pollutants (including food preservatives), poisonous substances & chemicals
- Age (young to middle aged dogs are the most commonly affected)
- Hormonal influences (particularly if a bitch is in season, in whelp or nursing puppies)
- Stress ~ for example, fireworks, thunderstorms, separation anxiety, whelping, etc.
- Diarrhoea (intermittent or persistent, with no obvious other cause)
- Depression & lethargy & the look of premature ageing
- Skin irritation or sores, nail bed problems, mouth ulcers, nose or anal lesions
- Bruising &/or bleeding from gums, nose, bowel or bladder
- Excessive drinking & urinating
- High temperature
- Weakness in the legs, muscle wastage (especially on top of head)
- A tendency to lameness ~ limping (with no obvious other cause)
- Anaemia (pale gums, tongue & eye rims)
- Collapse
- Intermittent symptoms that can disappear & reappear
- Ongoing symptoms that even after treatment remain constant & unresolved
WHAT ARE THE MOST COMMON AUTO-IMMUNE MEDIATED DISEASES?
AUTOIMMUNE HAEMOLYTIC ANAEMIA (AIHA or IMHA):
The body forms antibodies against its own red blood cells resulting in increased destruction of red blood cells which causes anaemia & sometimes jaundice. Common signs include listlessness, depression, unwillingness to exercise, or collapse.
IMMUNE-MEDIATED THROMBOCYTOPENIA (IMTP):
AUTOIMMUNE THYROIDITIS:
ADDISONS DISEASE (HYPOADRENOCORTICISM):
Initial symptoms can include stomach disturbances such as vomiting. Poor appetite can occur. Lethargy is also an early sign. These are pretty vague signs & it is extremely easy to miss this disease. More severe signs occur when the dog with the disease is stressed or when potassium levels in the blood get high enough to interfere with heart function.
KNOWN AS A 'CRISIS' WHICH CAN LEAD TO RAPID DEATH
Diagnosis is made by carrying out an ACTH response test - administration of this hormone should stimulate production of adrenal hormones. If this does not occur, hypoadrenocorticism is present.
IMMUNE MEDIATED POLYARTHRITIS (IMPA):
This can be a primary autoimmune disease or part of a multi-systemic disease such as 'Systemic Lupus Erythematosus' (SLE). It involves the synovial fluid in the joints of the dog, & diagnosis may be confirmed by joint fluid analysis.
SYSTEMIC LUPUS ERYTHEMATOSUS (SLE):
This is a multi-system autoimmune disease involving the skin, & which can also involve the heart, kidneys, or other autoimmune diseases such as IMPA, AIHA or IMTP (see above).
AUTOIMMUNE SKIN DISEASE:
There are many of these, & they can be either primary or secondary to other autoimmune diseases. Identification is by skin biopsy.
WHAT TREATMENT IS AVAILABLE FOR AUTOIMMUNE MEDIATED DISEASES?
Most AI diseases are treated with very high doses of corticosteroids or other immuno~suppressive drugs to lower the immune response. The type & duration of treatment will be based on each individual case. However, it is important to have a good support network around you, including your Vet as well as family & friends, as in many cases the ‘management' of the disease can be the most difficult aspect to deal with for both dog & owner.
All content copyright © 2015